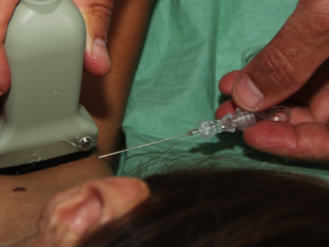
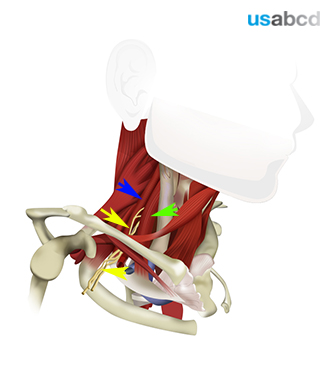
If the perineural spread of local anaesthetic is not perfect, the needle can be relocated in real-time before injection of the remaining local anaesthetic
Click on the VIDEO CLIP button to view the video
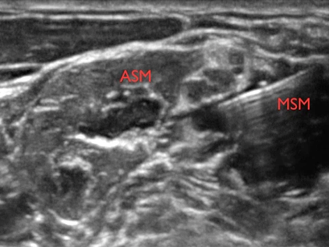
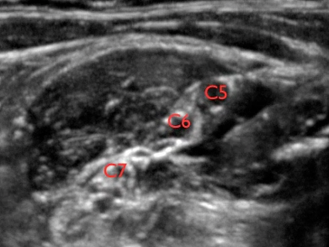
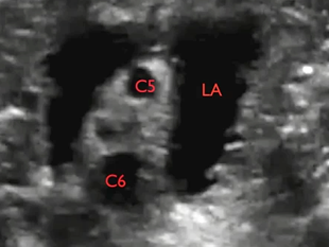
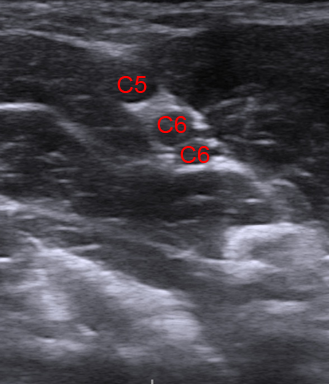
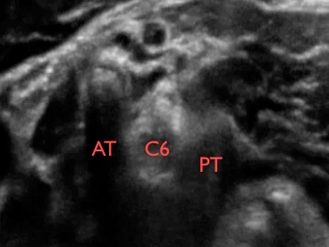
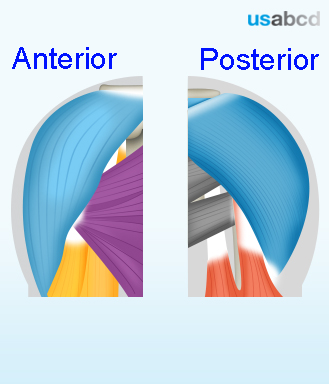
C5 = spinal nerve root of C5; C6 = spinal nerve root of C6 (2 profiles); ASM = anterior scalene muscle; MSM = middle scalene muscle