To evaluate the entire area at the sub diaphragmatic level, Morison’s pouch and anterior liver tip, sweep the transducer from the anterior to posterior position.
Here exemplified at the Morison’s pouch level.
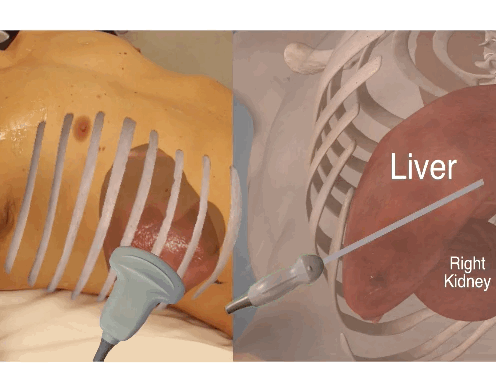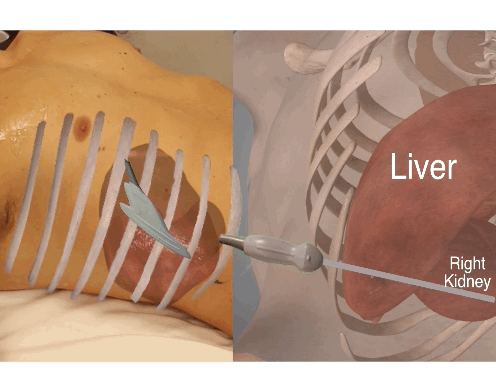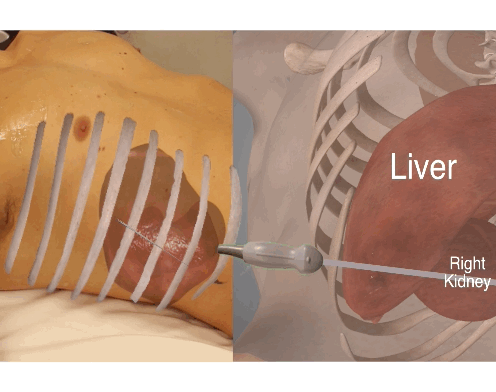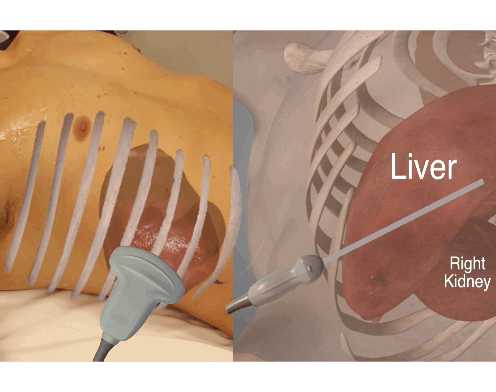
To evaluate the entire area at the sub diaphragmatic level, Morison’s pouch and anterior liver tip, sweep the transducer from the anterior to posterior position.
Here exemplified at the Morison’s pouch level.

Obtain the perihepatic view.
Look for free fluid between the diaphragm and the liver (subdiaphragmatic) – remember the sweep of the transducer from anterior to posterior position to evaluate the entire area of the hepato-diaphragmal area.
Look for free fluid between the liver and the kidney (Morison’s pouch) – – remember the sweep of the transducer from anterior to posterior position to evaluate the entire area of the hepato-renal recess.
Move the probe anteriorly and caudally to look for free fluid at the anterior tip of the liver and sweep again.
Intraperitoneal fluid appears as a black anechoic (black) area.
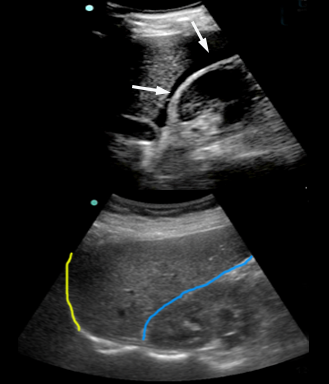
At the top free fluid (marked with white arrows) is seen in Morrison’s pouch and at the tip of the liver – the subdiaphragmatic area is not visualised in this image
Free fluid is seen as anechoic (black) areas in locations where fluid is not normally found.
Free fluid often collects in specific locations in the abdomen – these include:
Perihepatic:
• The hepatorenal recess (Morrison’s pouch) between the liver and the right kidney
• The space between the liver and right diaphragm (subdiaphragmatic)
• The anterior tip of the liver
Perisplenic:
• The splenorenal recess between the spleen and the left kidney
• The space between the spleen and left diaphragm
Pelvic:
• The rectouterine pouch, vesicouterine pouch, and around intestines in the female
• The rectovesical pouch and around the intestines in the male
Peri-intestinal:
• Between the intestines
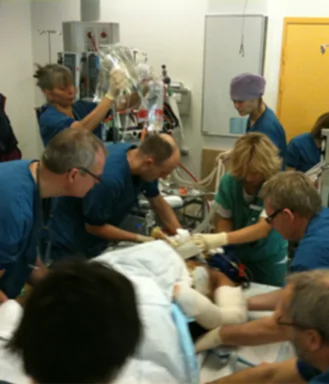
The original Focused Assessment with Sonography for Trauma (FAST) and the extended eFAST protocols were developed for assessment of trauma patients.
These address two concerns – pneumothorax and internal bleeding in the thorax or abdomen.
In Essential Emergency Ultrasonography we move away from the protocols towards a focused questions approach.
Ask a clinical question and answer it with all you have got – including the transducer.
We do recognise, however, that in the multi-trauma patient, the following questions your transducer can help you with are: does the patient have 1) a pneumothorax? 2) a hemothorax? 3) a hemopericardium? 4) an intraabdominal bleeding?
No. 1, 2 and 3 are covered by the previous lessons. In the following we only address no. 4 by answering the question “Is intraperitoneal free fluid visible?”
Always find the largest diameter.
When measuring the abdominal aortic, the largest diameter should be found.
An intramural thrombus is often seen with abdominal aortic aneurisms.
Thus, it is essential to measure the entire aorta – from outer edge to outer edge.
Tips
When a mural thrombus is present, the lumen of the aorta is narrowed (and is most often irregular and not circular) – remember to measure the entire aorta not just the lumen.
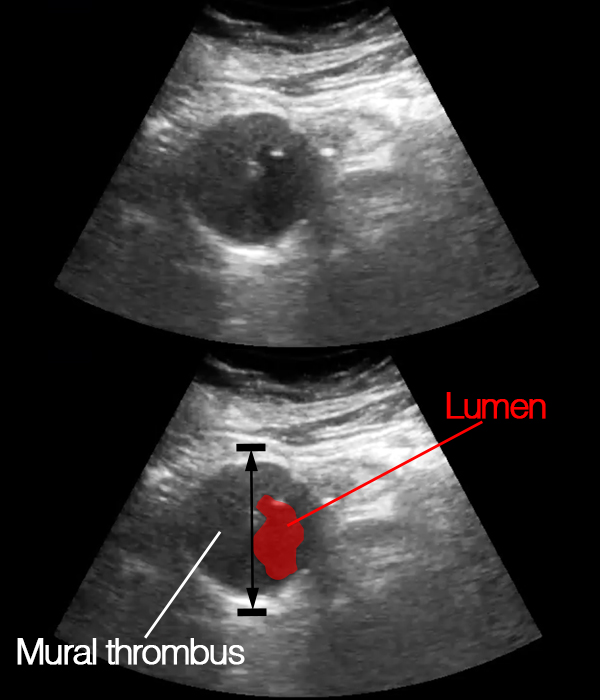
A maximum abdominal aortic diameter of <3.5 cm makes rupture very unlikely.
In a patient with the relevant symptoms and an abdominal aortic diameter >3.5 cm, a ruptured abdominal aortic aneurism is possible.
Most ruptures (90%) do however occur at maximum abdominal aortic diameters >5 cm.
Other findings supporting a clinical suspicion of ruptured abdominal aneurism:
– Free intraperitoneal fluid on focused ultrasonography of the abdomen (this is covered later in this lesson).
Rupture into the peritoneum is only seen in 20% of patients with rupture – rupture into the retroperitoneum is much more frequent (>75% of cases), but is difficult to asses using ultrasonography.
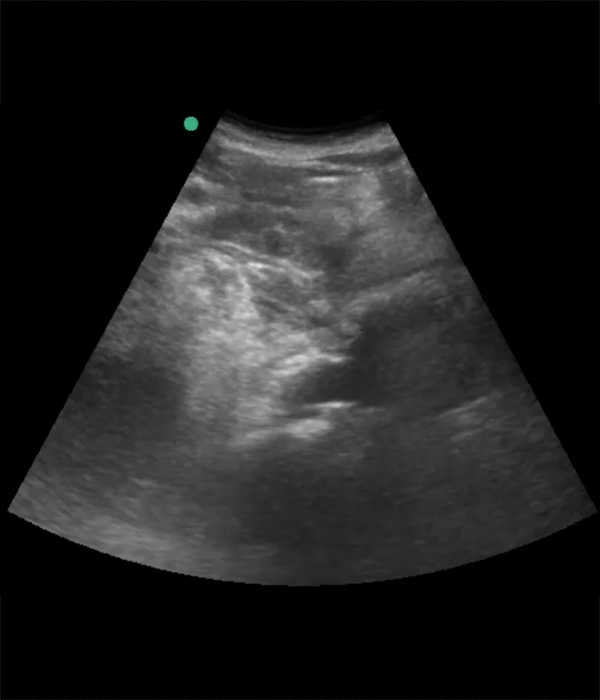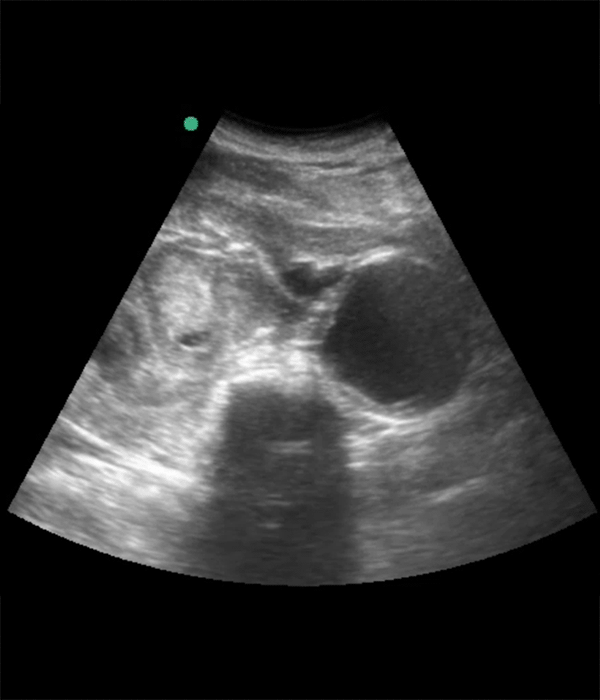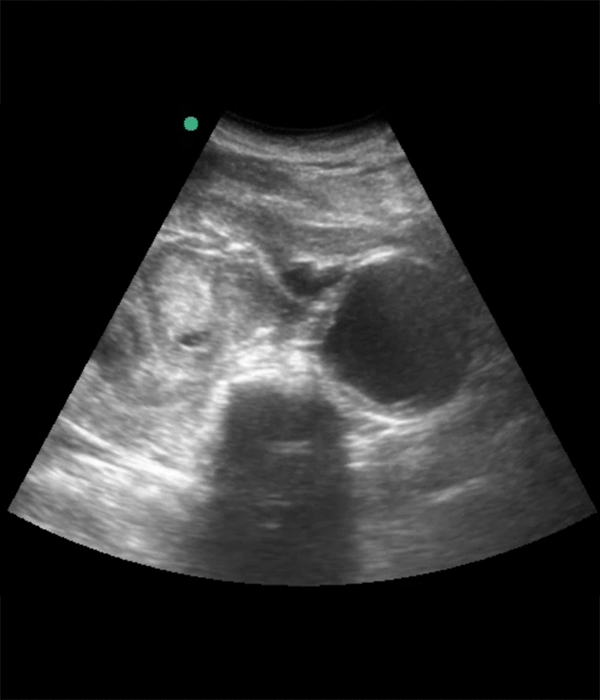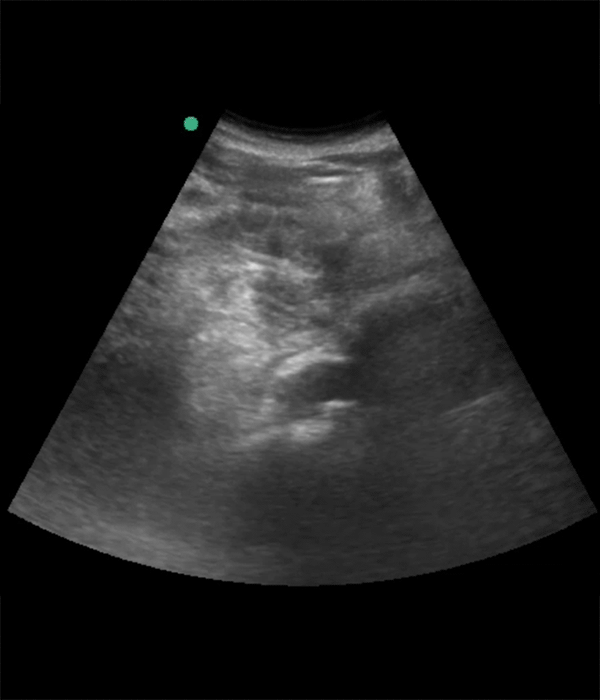
In adults, the normal largest abdominal aortic diameter is <3.5 cm
Above 3.5 cm, there is an exponentially increasing risk of rupture within the next 5 years with increasing maximal diameter size, but the size at rupture is >5.0 cm in 90% of cases.
Ruptured abdominal aortic aneurism is a clinical diagnosis – no ultrasonographic findings can rule out a ruptured aneurism.
However, the classical triad of pain, hypotension and pulsatile abdominal mass due to rupture is only seen in 25-50% of patients and ultrasonography may aid the diagnosis.
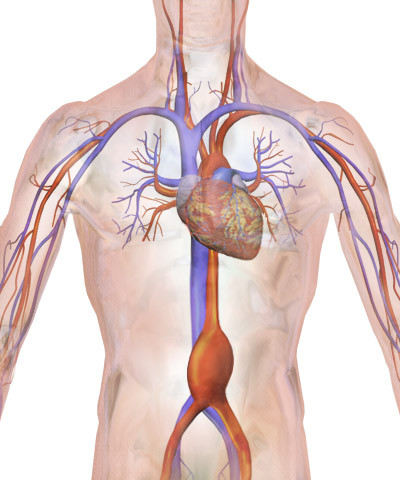
Illustration from: Blausen.com staff. “Blausen gallery 2014”. Wikiversity Journal of Medicine. DOI:10.15347/wjm/2014.010. ISSN 20018762
At this point, you should feel confident in how to obtain the abdominal views.
If you do not feel confident, please review the previous topics.
If you do feel confident – now move on to answering the focused questions.
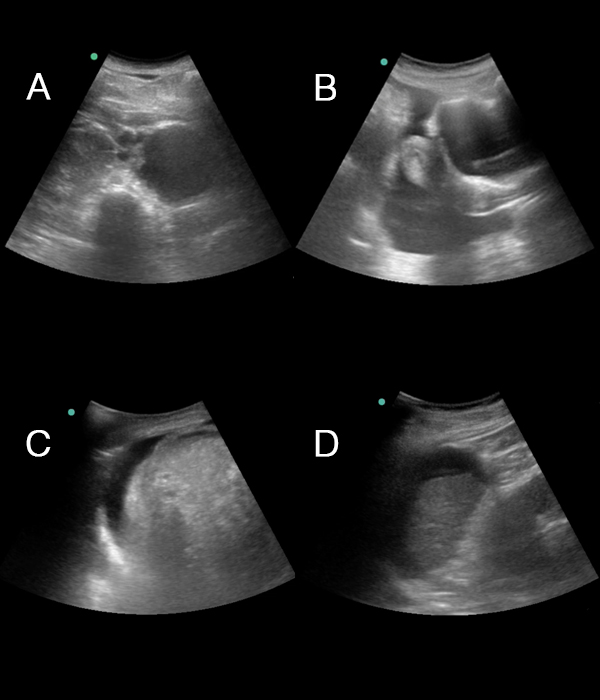
The focused questions in focused ultrasonography of the abdomen are:
• Is abdominal aortic aneurism/dissection present?
• Is free intraperitoneal fluid visible?
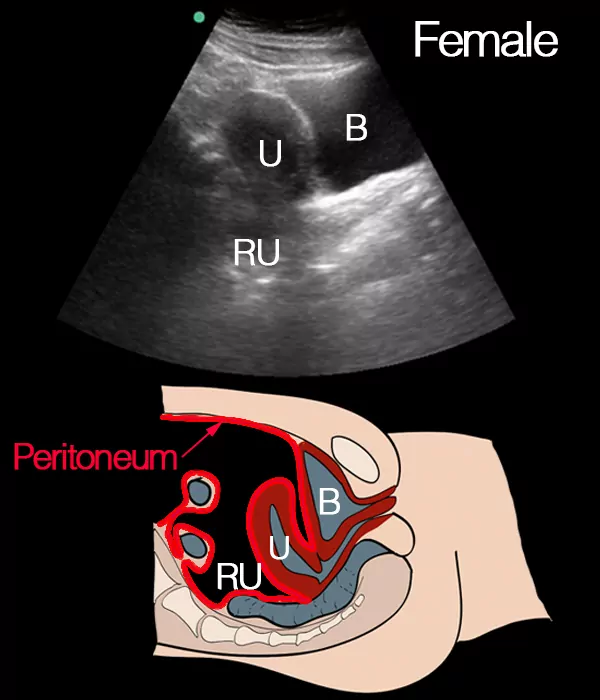
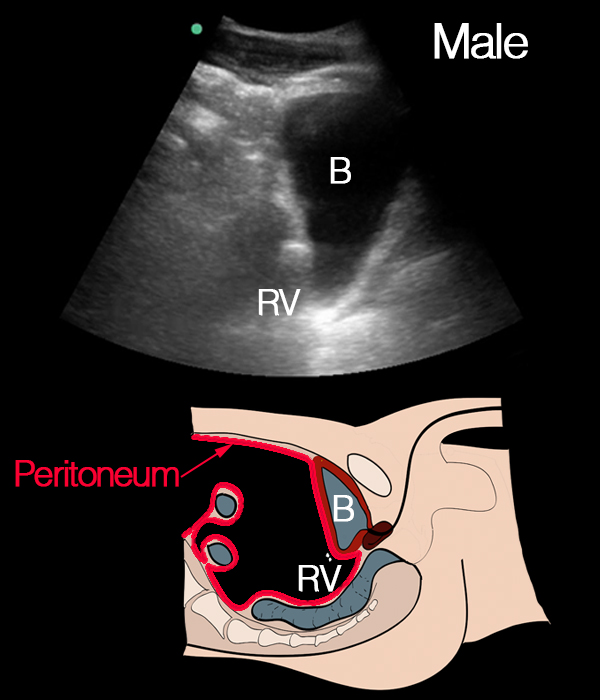
Intraperitoneal fluid does not only gather in the rectovesical pouch.
In men it can be seen either in the rectovesical pouch or surrounding the the intestines, or both.
Notice the peritoneum marked as a red line as its anatomy is important for understanding where to look for intraperitoneal fluid while scanning
Intraperitoneal fluid does not only accumulate in the rectouterine pouch.
In women ultrasonographic signs of fluid can be found in the rectouterine pouch, between the uterus and the bladder (vesicouterine pouch) or surrounding the intestines.
Notice the peritoneum (red line) as its anatomical location is important for understanding where to look for intraperitoneal fluid while scanning.