Description
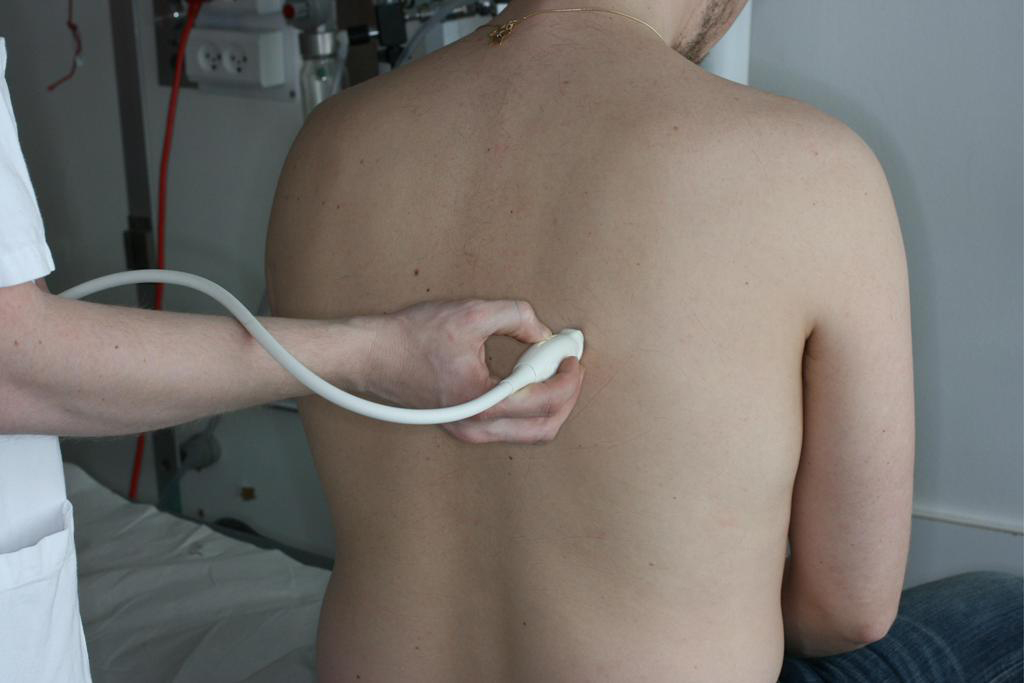
Lung ultrasound (LUS) is among the most innovative ultrasound applications. The latest developments in lung US are based on the interpretation of a few signs (mostly artefacts) rather than on technological advances.
The interest in lung ultrasound is growing fast and it is especially interesting to intensivists, emergency medicine physicians, anesthesiologists, and radiologists.
This e-learning program describes the clinical application of lung ultrasound in the evaluation of the critical care patient with respiratory problems.
You will learn how to:
- Choose the appropriate ultrasound system and probe for lung ultrasound imaging
- Identify lung and chest wall structures on the ultrasound 2D image (skin, muscle, intercostal space, pleura, diaphragm)
- Identify the ”bat-sign”
- Identify the basic sonography of 2D lung ultrasound: A-lines, B-lines, lung sliding, lung point and lung pulse
- Use M-mode imaging to identify the normal ”sea-shore” sign and the other characteristic air artefacts suggesting normal aeration pattern: A-lines with lung sliding and lung pulse
- Identify liver and diaphragm on lower right side of the thorax
- Identify spleen and diaphragm on lower left side of the thorax
- Identify pneumothorax
- Identify and characterize air artefacts to rule out pneumothorax: presence of lung sliding, lung pulse, and B-lines
- Identify and characterize findings typical of pneumothorax: presence of lung point (both with 2D imaging and M-mode)
- Identify pleural effusion
- Use lung-ultrasound imaging goal directed when evaluating the critical care patient